Dr. Dustin Clark, an Emergency Medicine specialist from Johnson City, is one of the medical directors at Smoky Mountain Home Health and Hospice. He took some time with us to answer important questions and provide valuable information about hospice care.
What is the difference between curative care and palliative or comfort care?
“A lot of confusion exists between palliative care, or comfort care, and curative care and how those things can be different.
The goals of curative care versus comfort care are different. When we talk about curative care, people are concerned with fixing the disease that is causing the problem. In comfort care we are not so much concerned with fixing the disease because frequently we can’t, but what we are concerned with is comfort of patients. Patients feeling as well as they can for as long as they can so they can enjoy a better quality of life.
People are fearful that being in hospice means that they have been assigned to dying very quickly which is certainly not the case. Often people are concerned that being in hospice means that no one is going to care for them anymore and that they are going to die very soon and nothing could be further from the truth.”
Do I have to be on morphine in hospice care?
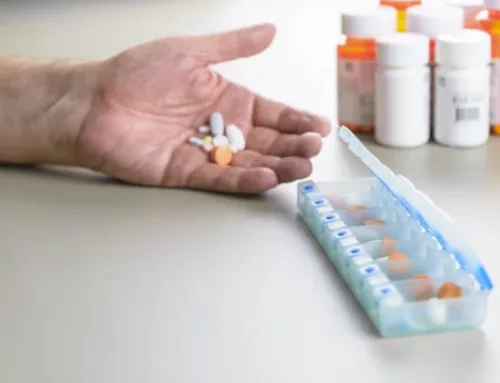
“Morphine is one of those drugs that has a particular stigma with it. We do use morphine at times when it is appropriate. I like to let people know that there is no set schedule, there’s no cookbook or formula that we follow. That doesn’t mean that as soon as you are on hospice that you start getting high-powered drugs and you are sedated for the rest of your life.
I talk with people about each individual being different and each individual case being different. Some people need more aggressive pain control in the beginning. We’ve certainly have had multiple hospice patients who never required any morphine at all. I think often times the negative experiences stick out in people’s minds.”
Do I have to have cancer to receive hospice care?
“Most people are familiar with cancer diagnoses and being admitted to hospice because of cancer. In fact, cancer is not the majority of the diagnoses that our patients have. They have all sorts of other issues that are in the final stages or at the end of life.
Trying to make a determination between when it is time to stop pursuing a cure for these things and move on to just trying to be comfortable, can be challenging at times. Essentially in most of those cases, congestive heart failure specifically, it’s really after all of the available treatments have been tried and the patient is still continuing to have symptoms and there is no chance for a cure. But there is a chance of making the patient more comfortable in hospice.”
How does hospice impact a patient’s quality of life?
“There are lots of differences that can occur depending on when patients become involved in hospice care. Traditionally you might think of it (quality of life) as patients being able to do more than they did in the past or somehow their disease process has lessened. And that may or not be the case in hospice.
Oftentimes, some of the things that get used in curative therapies can be very uncomfortable or at least very inconvenient for patients.
One of the things that is so freeing for people once they are involved in hospice care is really having a very supportive community and no longer is your world governed by schedules and appointments. Quality of life for the patient may not involve being in the hospital three out of four weeks every month or being in a doctor’s office for half a day most of the days of a week. We encourage people to make those decisions about what really is quality of life for each individual person.
In hospice we take a different approach where patients make their own decisions for as long as they are able.
Why are doctors uncomfortable with having the end of life talk?
“Honestly, there is not a great deal of education concerning palliative care and life care in typical medical training. I think in general, death has always been seen as the great enemy as it concerns modern medicine. In a lot of ways, having those talks means you have lost in some way.
But working in the hospice realm, you understand that there are many ways to measure success and to have victories in dealing with patients who are at a very vulnerable time in their life who really need the best care that is available.”